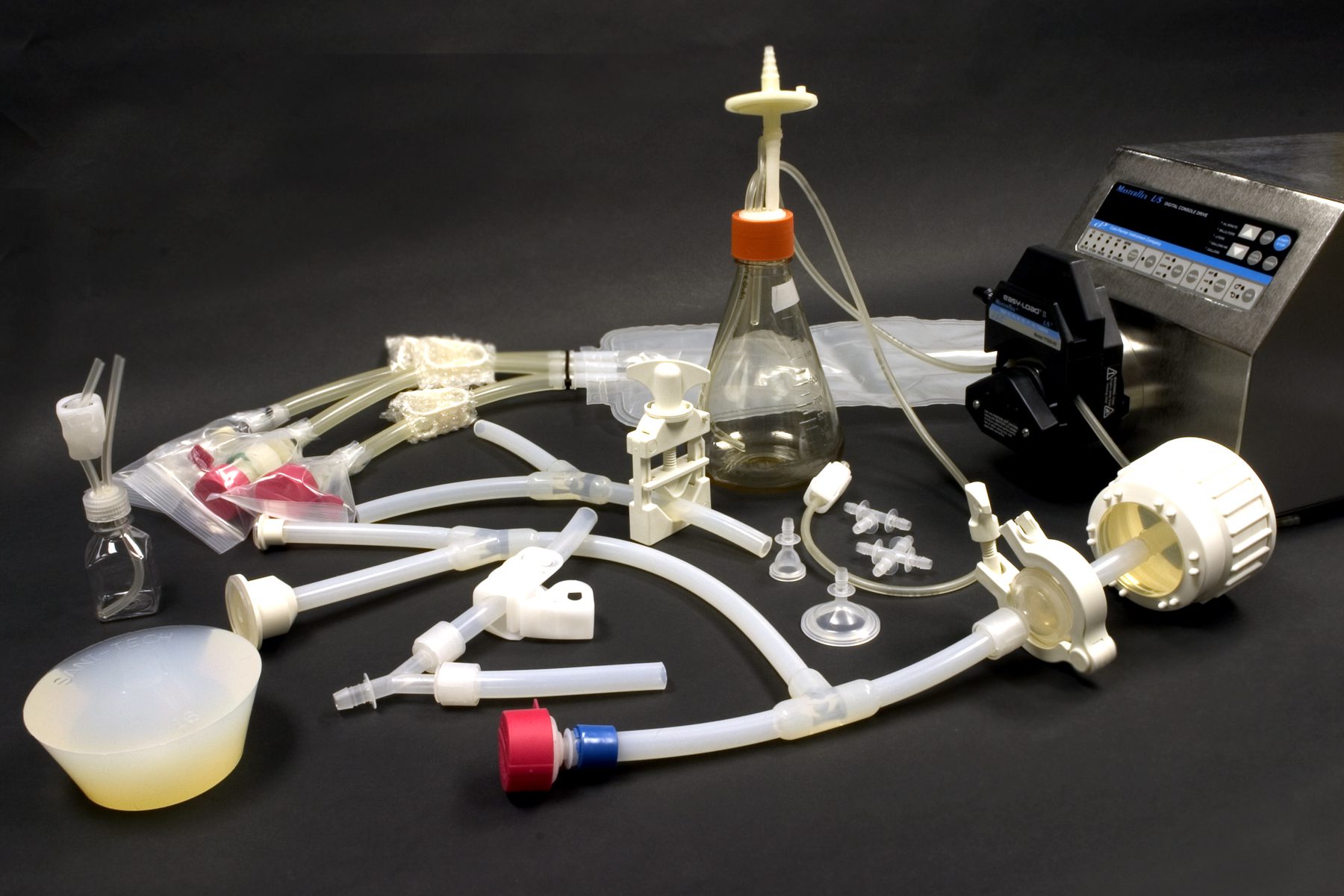
Validating a Single Use Process System- Sterility Claim vs. Microbial Control
As we’ve mentioned in this blog before, both at Holland and the rest of the biopharmaceutical process
industry, we’re seeing an increasing number of customers switching to disposable process equipment. This can be scary stuff for stainless guys. Customers, however, are finding safety, time, and cost reduction benefits compelling enough to switch to single use systems for applications ranging from buffer formulation and bulk intermediate, all the way to final fill. For many of these applications, microbial control or even sterility is required to ensure system safety and product purity. Today’s post will take a look at one of the most common sterilization methods for single use assemblies, gamma irradiation, and what standards and methods should be followed to call something “sterile”.
To begin understanding why and where a sterility claim may be needed, we need to look at to the origins of single use process equipment. Disposable products were first used in small scale lab applications where time and cost of stainless equipment was prohibitive. As these lab applications developed momentum and scale, there became a need for presterilized products that could be directly incorporated into critical process applications. In order to validate systems and ensure a sufficiently high probability of bioburden reduction and sterility, the bioprocessing industry has turned to standards established for the validation of sterilization of healthcare equipment by irradiation developed by organizations such as the American National Standards Institute (ANSI), the Association for the Advancement of Medical Instrumentation (AAMI), the International Organization for Standardization (ISO), the ASTM, and BPSA guidance.
We’ve talked about gamma irradiation as a means of sterilization in prior posts, so we will now turn our attention to the difference between sterility and microbial control. To be claimed as sterile, industry standards require, “validation of the efficacy and reproducibility of the sterilization process, based on determination of average bioburden and subsequent sterility testing of systems after minimal radiation exposure”. These systems are also subject to routine auditing that examines bioburden and sterility testing results. For prototype or lab systems, the process to make a sterile claim can be cost prohibitive. As an alternative to the sterile claim, many systems can be simply exposed to a sterilizing irradiation dose of 25 kGy and claimed as microbially controlled. In sum, components or systems requiring zero or low bioburden when applied to a nonsterile process, do not need to be validated as sterile, but simply validated as microbially controlled. We will spend the rest of this post helping explain when validated sterility is required or when microbial control is appropriate.
Let’s revisit the four basic stages we can divide biopharmaceutical manufacturing into. First, we have “upstream” processing where we mix nutrients and producer cells in a fermenter or bioreactor allowing the cells to produce the target molecule. Next, we go to the harvest stage where cells are separated from the target molecule using methods like filtration and centrifugation. Third is downstream processing where a series of separation, purification, and chromatography steps produce a purified bulk drug product. Finally, we have the formulation and fill stage where the purified bulk is sterile filtered and aseptically filled into containers. This final stage is similar to how synthetic pharmaceuticals are manufactured aseptically.
Through all of these stages, it is important to prevent any unwanted microbial contamination. What degree of control is driven by the end user and international regulations which dictate that products and processes claimed as sterile must be validated to prove sterility. What constitutes a validated sterile process? Validation is by definition, “the process of establishing documented evidence that provides a high degree of assurance that a specific process will consistently produce a product meeting its predetermined specifications and quality attributes”. A sterile process, then, is a validated method of sterilizing a product such that the sterility assurance level (SAL) is less than or equal to 10-6 (one in a million!). These regulations do not, however, apply processes claimed as microbially controlled, which also may have zero or low bioburden but have not been validated with a defined SAL. What this means in respect to the bioprocessing steps described above is while the assurance of validated sterility is necessary for bulk drug product and final fill single use systems, preparative stages after which product will undergo additional refining (i.e. sterile filtration) can be operated under the tight microbial control afforded by irradiation.
If it is determined that a process must be validated as sterile, there are a few methods most commonly employed. First, we need to figure out what to test. In applications where a single use system is used, it is common that multiple variations of a system are used in a process. In these applications, it is often only necessary to validate a single product from a family known as a “Master Product”. The Master Product is usually the largest product in a family, but it can also be the product which possesses the most components, the greatest number of materials, or even the one that requires the most handling during manufacture. Simulated or equivalent products may also be used. For more information on what equivalent and similar products are, please refer to the BPSA’s guidance on sterilization and validation of single use process systems.
Once we’ve determined which product to test, we need to determine what part of the product needs to be tested. If you’ve used single use processing systems in the past, you know how large these can be and can imagine how difficult it can be quantify bioburden and sterility. In some cases, it is only necessary to test and validate the fluid path. Because the system (ie tubing, bags, ect) can act as its own barrier to contamination, we avoid having to test the entire product and avoid the issue of handling its external surfaces without contamination. Large products can also be sectioned, or split into parts that are easier to test. Each section is then tested and summed to come up with the bioburden of the entire bag.
To test the bioburden of a fluid path or sectioned product, we will partially fill the system with sterile buffer, ensuring all surfaces are wetted, then agitate the article by hand to promote suspension of organisms. The buffer is then removed and tested using standard microbiological methods. Sterility testing is accomplished by a similar method, but a growth media is used in lieu of sterile buffer.
As you can probably tell, validating sterility is anything but quick and easy. Determining whether a process needs to be validated as sterile or microbially controlled is critical in optimizing time and cost requirements for a project, considerations which are ultimately borne by the biopharmaceutical manufacturer. While disposable process equipment offers significant advantages to manufacturers, they are not without significant decisions to be made by all stakeholders. While some applications may only require microbial control, sterile processes must be validated as such. While we covered a lot of ground, the purpose of this post is to help distinguish between sterile and microbial controlled, provide an overview of the sterilization validation process, and discuss where these needs fit into the overall biopharmaceutical manufacturing process. For more questions about your specific application, contact a Holland Sales Engineer today!